Evaluación del estrés oxidativo asociado a la alteración de la homeostasis Tiol/Disulfuro en gatos con infección por Coronavirus felino
Resumen
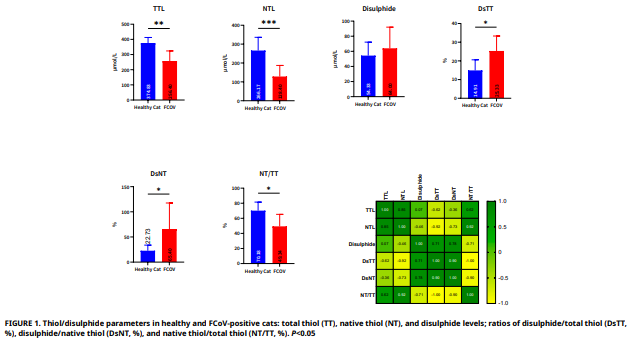
Este estudio evaluó la homeostasis tiol/disulfuro y su relación con el estrés oxidativo en gatos diagnosticados con infección por coronavirus felino. La población del estudio estuvo compuesta por 18 gatos, incluidos 11 animales positivos para coronavirus felino y 7 controles clínicamente sanos. Las concentraciones séricas de tiol total, tiol nativo y disulfuro se determinaron mediante un método espectrofotométrico. En comparación con los controles sanos, los gatos coronavirus felino-positivos presentaron concentraciones significativamente más bajas de tiol total y tiol nativo, lo que indica una reducción marcada de la capacidad antioxidante basada en tioles. De manera paralela, se observó un desplazamiento del equilibrio redox hacia la formación de disulfuros, reflejado por una disminución pronunciada de la relación tiol nativo/tiol total. Estas alteraciones sugieren una depleción del pool de tioles bajo condiciones de aumento de la carga oxidativa. En conjunto, la alteración de la homeostasis tiol/disulfuro parece estar estrechamente asociada con el estrés oxidativo durante la infección por coronavirus felino y podría contribuir a la patogénesis de la enfermedad. Los hallazgos del presente estudio aportan información relevante sobre los mecanismos bioquímicos subyacentes al daño oxidativo en gatos infectados con coronavirus felino y respaldan la posible utilidad de los parámetros tiol/disulfuro como indicadores tempranos de estrés oxidativo, con potenciales implicaciones para futuras estrategias terapéuticas basadas en antioxidantes.
Descargas
Citas
Pedersen NC. A review of feline infectious peritonitis virus infection: 1963-2008. J. Feline Med. Surg. [Internet]. 2009; 11(4):225-258. doi: https://doi.org/fjg9k5 DOI: https://doi.org/10.1016/j.jfms.2008.09.008
Gao YY, Wang Q, Liang XY, Zhang S, Bao D, Zhao H, Li SB, Wang K, Hu GX, Gao FS. An updated review of feline coronavirus: mind the two biotypes. Virus Res. [Internet]. 2023; 326:199059. doi: https://doi.org/grq9dr DOI: https://doi.org/10.1016/j.virusres.2023.199059
Mohseni N, Royster A, Ren S, Ma Y, Pintado M, Mir M, Mir S. A novel compound targets the feline infectious peritonitis virus nucleocapsid protein and inhibits viral replication in cell culture. J. Biol. Chem. [Internet]. 2023; 299(3):102976. doi: https://doi.org/qzv5 DOI: https://doi.org/10.1016/j.jbc.2023.102976
Christopher MM, Broussard JD, Peterson ME. Heinz body formation associated with ketoacidosis in diabetic cats. J. Vet. Intern. Med. [Internet]. 1995; 9(1):24-31. doi: https://doi.org/bg8qw8 DOI: https://doi.org/10.1111/j.1939-1676.1995.tb03268.x
Harvey JW, Kaneko JJ. Mammalian erythrocyte metabolism and oxidant drugs. Toxicol. Appl. Pharmacol. [Internet]. 1977; 42(2):253-261. doi: https://doi.org/d9zj7j DOI: https://doi.org/10.1016/0041-008X(77)90002-3
Wolfe LG, Griesemer RA. Feline infectious peritonitis. Pathol. Vet. [Internet]. 1966; 3(3):255-270. doi: https://doi.org/ffgfgg DOI: https://doi.org/10.1177/030098586600300309
Betteridge DJ. What is oxidative stress? Metabolism [Internet]. 2000; 49(2 Suppl 1):3-8. doi: https://doi.org/d99s42 DOI: https://doi.org/10.1016/S0026-0495(00)80077-3
Suresh DR, Annam V, Pratibha K, Prasad BM. Total antioxidant capacity-a novel early biochemical marker of oxidative stress in HIV-infected individuals. J. Biomed. Sci. [Internet]. 2009; 16:61. doi: https://doi.org/bzfxbb DOI: https://doi.org/10.1186/1423-0127-16-61
Pizzino G, Irrera N, Cucinotta M, Pallio G, Mannino F, Arcoraci V, Squadrito F, Altavilla D, Bitto A. Oxidative stress: harms and benefits for human health. Oxid. Med. Cell. Longev. [Internet]. 2017; 2017:8416763. doi: https://doi.org/gkgcv7 DOI: https://doi.org/10.1155/2017/8416763
Tecles F, Caldín M, Tvarijonaviciute A, Escribano D, Martínez-Subiela S, Cerón JJ. Serum biomarkers of oxidative stress in cats with feline infectious peritonitis. Res. Vet. Sci. [Internet]. 2015; 100:12-17. doi: https://doi.org/f7f9xw DOI: https://doi.org/10.1016/j.rvsc.2015.02.007
Kayar A, Dokuzeylül B, Kandemir FM, Kırbaş A, Bayrakal A, Or ME. Total oxidant and antioxidant capacities, nitric oxide and malondialdehyde levels in cats seropositive for feline coronavirus. Vet. Med. [Internet]. 2015; 60(5):274-281. doi: https://doi.org/qzv6 DOI: https://doi.org/10.17221/8180-VETMED
Erel O, Neselioğlu S. A novel and automated assay for thiol/ disulphide homeostasis. Clin. Biochem. [Internet]. 2014; 47(18):326-332. doi: https://doi.org/f6r6dk DOI: https://doi.org/10.1016/j.clinbiochem.2014.09.026
Frijhoff J, Winyard PG, Zarkovic N, Davies SS, Stocker R, Cheng D, Knight AR, Taylor EL, Oettrich J, Ruskovska T, Gasparovic AC, Cuadrado A, Weber D, HE Poulsen, Grune T, Schmidt HHHW, Ghezzi P. Clinical relevance of biomarkers of oxidative stress. Antioxid. Redox Signal. [Internet]. 2015; 23(14):1144-1170. doi: https://doi.org/f7z26x DOI: https://doi.org/10.1089/ars.2015.6317
Değirmençay Ş, Çamkerten G, Çamkerten İ, Aktaş MS. Investigation of thiol/disulphide homeostasis and ischemia-modified albumin levels in dogs with canine distemper. Vet. Arhiv. [Internet]. 2021; 91(1):39-49. doi: https://doi.org/qzv8 DOI: https://doi.org/10.24099/vet.arhiv.0867
Adıgüzel S, Merhan O. Determination of thiol/disulfide homeostasis and oxidative stress index in sheeppox virus. Anim. Health Prod. Hyg. [Internet]. 2024; 13(2):21-25. doi: https://doi.org/qzv9 DOI: https://doi.org/10.53913/aduveterinary.1534512
Şenel Y, Terzi OS, Kara E, Erel O, Neşelioğlu S, Ceylan E. Alterations in serum thiol-disulfide homeostasis in clinical canine parvoviral enteritis. Turk. J. Vet. Anim. Sci. [Internet]. 2024; 48(2):88-96. doi: https://doi.org/qzwb DOI: https://doi.org/10.55730/1300-0128.4341
Addie D, Belák S, Boucraut-Baralon C, Egberink H, Frymus T, Gruffydd-Jones T, Hartmann K, Hosie MJ, Lloret A, Lutz H, Marsilio F, Pennisi MG, Radford AD, Thiry E, Truyen U, Horzinek MC. Feline infectious peritonitis ABCD guidelines. J. Feline Med. Surg. [Internet]. 2009; 11(7):594-604. doi: https://doi.org/fsrxcs DOI: https://doi.org/10.1016/j.jfms.2009.05.008
Sherding RG. Feline infectious peritonitis (feline coronavirus). In: Birchard SJ, Sherding RG, editors. Saunders manual of small animal practice. 3rd ed. [Internet]. St. Louis (MO, USA): Saunders Elsevier. 2006; p. 132-143. doi: https://doi.org/fm5598 DOI: https://doi.org/10.1016/B0-72-160422-6/50012-7
Thayer V, Gogolski S, Felten S, Hartmann K, Kennedy M, Olah GA. 2022 AAFP/EveryCat feline infectious peritonitis diagnosis guidelines. J. Feline Med. Surg. [Internet]. 2022; 24(9):905-933. doi: https://doi.org/qswn DOI: https://doi.org/10.1177/1098612X221118761
Tasker S, Addie DD, Egberink H, Hofmann-Lehmann R, Hosie MJ, Truyen U, Belák S, Boucraut-Baralon C, Frymus T, Lloret A, Marsilio F, Pennisi MG, Thiry E, Möstl K, Hartmann K. Feline infectious peritonitis: European Advisory Board on Cat Diseases guidelines. Viruses [Internet]. 2023; 15(9):1847. doi: https://doi.org/gs535j DOI: https://doi.org/10.3390/v15091847
Tasker S. Diagnosis of feline infectious peritonitis: Update on evidence supporting available tests. J. Feline Med. Surg. [Internet]. 2018; 20(3):228-243. doi: https://doi.org/gr9kjx DOI: https://doi.org/10.1177/1098612X18758592
Felten S, Hartmann K. Diagnosis of feline infectious peritonitis: A review. Viruses. [Internet]. 2019; 11(11):1068. doi: https://doi.org/gj9tvp DOI: https://doi.org/10.3390/v11111068
Erdoğan H, Çamkerten İ, Çamkerten G, Ural K, Erdoğan S, Gunal I, Erel O. Effect of hot-iron disbudding on thiol-disulphide homeostasis in calves. Kafkas Univ. Vet. Fak. Derg. [Internet]. 2019; 25(3):335-339. doi: https://doi.org/qzwn
Cengiz HB, Gökçe Hİ. Investigation of the effects of feline coronavirus (FCoV)/FIP on calcium metabolism in cats. Mehmet Akif Ersoy Univ. Vet. Fak. Derg. [Internet]. 2021; 6(3):127-132. doi: https://doi.org/qzwp DOI: https://doi.org/10.24880/maeuvfd.970374
Ates I, Altay M, Yilmaz FM, Topcuoglu C, Neselioglu S, Erel O, Yilmaz N. Dynamic thiol/disulfide homeostasis in patients with autoimmune subclinical hypothyroidism. Endocr. Res. [Internet]. 2016; 41(4):343-349. doi: https://doi.org/qzwq DOI: https://doi.org/10.3109/07435800.2016.1156124
Şekeroğlu MR, Çokluk E, Yaylacı S, Erdem AF, Tuncer FB, Dheir H, Güçlü E, Öğütlü A, Çekiç D, Aydın A, Cinemre FBS. Thiol-disulphide homoeostasis in COVID-19: evaluation of its relationship with complete blood count parameters. Konuralp Med. J. [Internet]. 2021; 13(S1):460-467. doi: https://doi.org/qzwr DOI: https://doi.org/10.18521/ktd.917364
Tarhan M, Değer Y, Oğuz B, Özdek U. Investigation of thiol-disulphide homeostasis, total oxidant-antioxidant and ischemia-modified albumin levels in dogs with babesiosis. Alex. J. Vet. Sci. [Internet]. 2023; 77(1):21-29. doi: https://doi.org/qzzm DOI: https://doi.org/10.5455/ajvs.145761
Karaoğlanoğlu S, Erdal H. Thiol/disulphide homeostasis as a new oxidative stress marker in patients with COPD. Diagnostics [Internet]. 2025; 15(20):2584. doi: https://doi.org/qzzn DOI: https://doi.org/10.3390/diagnostics15202584
Bölükbaşı L, Merhan O. Lipid peroxidation and thiol/disulfide homeostasis in cattle with trichophytosis. Dicle Univ. Vet. Fak. Derg. [Internet]. 2024; 17(2):161-164. doi: https://doi.org/qzzp DOI: https://doi.org/10.47027/duvetfd.1534484
Shuid AN, Safi N, Haghani A, Mehrbod P, Haron MSR, Tan SW, Omar AR. Apoptosis transcriptional mechanism of feline infectious peritonitis virus infected cells. Apoptosis [Internet]. 2015; 20(11):1457-1470. doi: https://doi.org/f7sh9q DOI: https://doi.org/10.1007/s10495-015-1172-7
Pugliese M, Sfacteria A, Oliva G, Falcone A, Gizzarelli M, Passantino A. Clinical significance of R-OOHS, OXY, SHp and HMGB-1 in canine leishmaniasis. Animals [Internet]. 2021; 11(3):754. doi: https://doi.org/qzzq DOI: https://doi.org/10.3390/ani11030754
Kurtdede E, Taşkın N, İspir ES, Gülendağ E. The relationship between lipid profile, oxidative stress and thiol-disulfide levels in healthy, overweight and obese cats. Vet. Sci. Pract. [Internet]. 2024; 19(3):148-154. doi: https://doi.org/qzzr DOI: https://doi.org/10.17094/vetsci.1499578
Yeşilırmak N, Saritas O, Kurt B, Neselioglu S, Aktas A, Erel O. Investigation of thiol/disulfide homeostasis and clinical parameters in rosacea patients according to skin subtypes. J. Clin. Med. [Internet]. 2024; 13(14):4052. doi: https://doi.org/qzzs DOI: https://doi.org/10.3390/jcm13144052
Özgöçer T, Çelik H, Ceylan MR. Dynamic thiol-disulfide homeostasis post-COVID-19 depends on age, gender, and symptom severity. Cureus [Internet]. 2024; 16(10): e72097. doi: https://doi.org/qzzt DOI: https://doi.org/10.7759/cureus.72097
Aydın Ö, Özkurt G, Camkerken I, Eren E, Yanar KE, Aktaş MS. Investigation of ischemia-modified albumin and thiol/ disulfide homeostasis for the determination of oxidative stress in sheep with toxoplasmosis. Small Rumin. Res. [Internet]. 2023; 225:107023. doi: https://doi.org/qzzV DOI: https://doi.org/10.1016/j.smallrumres.2023.107023
Ulrich K, Jakob U. The role of thiols in antioxidant systems. Free Radic. Biol. Med. [Internet]. 2019; 140:14-27. doi: https://doi.org/gphk97 DOI: https://doi.org/10.1016/j.freeradbiomed.2019.05.035
Öztürk M, Özkan Y, Yalın-Sapmaz Ş, Erdal S, Taneli F, Kandemir H. Thiol-disulfide homeostasis: a potential new peripheral biomarker in adolescent depression. Psychiatry Clin. Psychopharmacol. [Internet]. 2024; 34(1):29-37. doi: https://doi.org/qzzw DOI: https://doi.org/10.5152/pcp.2024.23744
Ertürk C, Altay MA, Büyükdoğan H, Çalışkan G, Erel Ö. Thiol/ disulfide homeostasis as a novel indicator of oxidative stress during the treatment process of patients with septic arthritis. Jt. Dis. Relat. Surg. [Internet]. 2020; 31(3):502-508. doi: https://doi.org/qzzx DOI: https://doi.org/10.5606/ehc.2020.71982
Baştan İ, İrdem Dİ, Sel T, Kaya-Kartal Y, Ergin SH, Tunç AS. Oxidative stress in neurological feline infectious peritonitis: cerebrospinal fluid 8-hydroxy-2'-deoxyguanosine and superoxide dismutase levels. Kafkas Univ. Vet. Fak. Derg. [Internet]. 2025; 31(4):547-556. doi: https://doi.org/qzz2 DOI: https://doi.org/10.9775/kvfd.2025.34251
Kasra F, Pourtaghi H, Yasini SP, Sarabandi S. Assessment of oxidative stress biomarkers in felines infected with calicivirus. Arch. Razi Inst. [Internet]. 2025; 80(2):383-388. doi: https://doi.org/qzz3 DOI: https://doi.org/10.32592/ARI.2025.80.2.383